Cornell Scale for Depression in Dementia: Study of Residents in a Northern Thai Long-Term Care Home
Article information
Abstract
Objective
This study aimed to analyse the validity of the Thai version of the Cornell Scale for Depression in Dementia (CSDD) when using DSM-IV criteria.
Methods
A cross-sectional study was carried out of 84 elderly residents in a residential care home setting in Thailand. The participants went through a comprehensive geriatric assessment which included a Mini-Mental State Examination, a Mini-International Neuropsychiatric Interview (MINI) and use of the CSDD tool. A ROC analysis was performed in order to test the validity of the CSDD as against the DSM-IV when used by the MINI.
Results
ROC analysis revealed a better score for those areas found under the curve for the CSDD-as against the DSM-IV criteria (0.96). With a cut-off score of >6, the CSDD yielded the highest sensitivity score (100%), plus produced a specificity of 81% and a negative predictive value of 100%. It also had a positive predictive value of 69%. The validity of the CSDD was found to be better for the group experiencing cognitive impairment than with the non-cognitive impairment group in terms of the agreement of CSDD items between patients and caregivers. The CSDD yielded a high internal consistency (Cronbach's alpha=0.87).
Conclusion
CSDD is a valid tool to use for identifying depressive disorders among Thai LTC home residents - those experiencing and those not experiencing cognitive impairment.
INTRODUCTION
Depression is commonly found among long-term care (LTC) home residents, though its prevalence varies,1,2 with some studies finding rates of up to nearly 90%.3-5 The inability to detect depression in nursing homes, and particularly among residents with dementia, is common;6,7 for example, Cohen et al.8 found in their study that less than 25% of depression cases are identified and treated in such settings. When diagnosing depression, one must be aware that the condition can be affected, not only by the age and gender of the respondents, but also by the environment they live in (even when the same measurement is used);1,9 therefore, the use of measures suited to specific populations and particular settings, such as long term care facilities, needs to be considered. In addition, there is strong evidence to suggest that language differences can cause differences in the factor structures of the measures used, and particularly among self-reporting tools.10
When attempting to screen for depression, the Cornell Scale for Depression in Dementia (CSDD)11 is considered one of the best tools to use with cognitively impaired patients, and is thus widely used in LTC facilities. The introduction of mandatory screening with the CSDD has been shown to increase the proportion of depressed dementia patients receiving anti-depressants from 20% (with no screening) to 44%.8 The validity of the CSDD tool has been investigated and substantiated, including cross-culturally.11-16
In terms of the validity of the CSDD, there have been two sets of results among the studies carried out thus far. The first set of studies has yielded a moderate level of accuracy - with an Area Under Curve (AUC) figure of around 0.70 to 0.80. For example, the studies of Leontjevas et al. reported an AUC figure of 0.76 for Provisional Criteria for Depression in Alzheimer's Disease (PCD-dAD) among patients with early-on-set dementia and also among proxy informants,12,13 which corresponds with the results of Barca et al.17 and Watson et al.,18 who examined the validity of the CSDD among patients in LTC homes. Another set of studies has yielded a higher level of accuracy, with an AUC score of 0.90 or more. For example, Kørner et al.19 reported an AUC of 0.98 to 0.99, while Schreiner and Maixner et al.20 reported an AUC of 0.90. Barca et al. argued that this difference was due to how strictly each study followed the assessment protocols suggested by Jaeschke et al.17,21 Among the Thai elderly, the validity and reliability of the CSDD have never been studied; therefore, the aim of our study was to test the performance of the Thai version of the CSDD against standard diagnoses, using clinician-rated DSM-IV criteria for major depressive disorder (MDD).
METHODS
Participants and procedures
The project was approved by the Ethics Committee at the Faculty of Medicine, Chiang Mai University, and was conducted as a cross-sectional study. All subjects in the LTC were invited to participate, including the caregivers (nurses). Those who did not participate had active physical or psychiatric diseases that meant they were unable to communicate effectively, a situation which would have proved an obstacle to the interview process. As a result, they were excluded.
Data were collected between March 2011 and June 2011. Of the 111 residents in the LTC invited to participate in the study, 84 agreed to participate, and informed consent was obtained from all of them. The participants included 84 patients of 60 years-of-age and over residing in an LTC home in northern Thailand, as well as 5 caregivers. A trained research nurse initially performed a diagnostic interview, in order to carry out a psychiatric diagnosis and to assess cognitive functions, using the Thai version of the Mini-International Neuropsychiatric Interview (MINI) tool - version 5.0,22 plus the Mini-Mental State Examination Thai 2002 instrument (MMSE Thai 2002).23 Both a patient and caregiver CSDD were employed by the research nurse, and both the caregivers and the patients were unaware of each others' scores.
Instruments
The MINI
The Mini-International Neuropsychiatric Interview (MINI) instrument, developed by Sheehan,24 was employed here as the standard for diagnosing DSM IV major depression,1,25,26 with the Thai version validated by Kittiratanapaiboon et al.27 The Thai version has kappa ranges of between 0.27 and 0.87 - showing the presence or otherwise of depressive disorders. In this study, the MINI and CSDD assessments were carried out 'blind' and independent of each other.
MMSE-Thai 2002
Cognitive impairment is a condition that affects a person's ability to think, concentrate, develop ideas, reason and remember, and when it develops with age is called dementia, though it can occur at any age.28 To measure the level of cognitive impairment among the participants in this study, the Mini-Mental State Examination (MMSE) was used, based on an original version used by Folstein et al.23,29 The highest score possible is 30, and the cut-off score in relation to the presence of cognitive impairment or dementia among elderly subjects depends on their level of education. For those who have completed elementary schooling, the cut-off score is 22 (out of 30); for those who have not it is 17 (out of 30) and for those who are illiterate, it is 14 (out of 23).
Cornell Scale for Depression in Dementia
The CSDD instrument was developed by Alexopoulos et al.,30 based on a review of the literature into depression among elderly patients and on a questionnaire completed by geriatric psychiatrists. It is used to rate the symptoms of depression found in an individual with dementia and contains nineteen questions, each of which can be given a score ranging from 0 (absent) to 2 (severe), or the score 'symptoms not possible to evaluate'. The scale is divided into five sub-scales, these being: 1) 'mood-related signs' (anxiety, sadness, a minimal reaction to pleasant events and irritability), 2) 'behavioral disturbance' (agitation, psychomotor retardation, multiple physical complaints and loss of interest), 3) 'physical signs' (loss of appetite, weight loss and lack of energy), 4) 'cyclic functions' (diurnal variation in mood, difficulty falling asleep, multiple awakening during the night and early morning awakening), and 5) 'ideational disturbance' (suicidal tendencies, low self-esteem, pessimism and mood-congruent delusions). The tool's internal consistency/reliability has been found to range from 0.76 to 0.84, and has shown a high level of correlation (r=0.96) with the diagnoses given by psychiatrists.30
Thai version of the CSDD
The author (NW) was granted permission by the developer to translate the CSDD into Thai, following the translation and cultural adaptation method, a process which involved an initial translation into Thai by a geriatric psychiatrist (NW), then a backward translation into English by a bilingual translator (a university professor) who had no prior knowledge of the questionnaire. The two versions produced were then assessed and compared item by item by the authors and the bilingual translator. The resulting final draft was then field tested with depressed elderly patients in a geriatric outpatient clinic - those not involved with the research project. A Cornell Scale assessment was carried out by a trained psycho-geriatric research nurse, who interviewed each patient and caregiver within a day of the depression being diagnosed by the MINI scale.
Data analysis
Means and standard deviations were used, and when comparing the two groups, either an unpaired t-test or a Mann-Whitney test was adopted, as appropriate. The test performances of the CSDD were evaluated for both the cognitively impaired and cognitively intact groups, were determined by comparing the MMSE score for each participant with their indi-vidual cut-off score - based on their level of education, and then examined using receiver operating characteristics (ROC) analyses of the sensitivity, specificity, positive predictive values (PPV) and negative predictive values (NPV) found. Point estimates and 95% confidence intervals (CIs) were computed to assess test performance characteristics across the different cut-offs and against the gold standard external diagnostic measure. To find the best cut-off score, the Youden index J was used. SPSS v. 17 (SPSS, Inc, USA) and MedCalc v. 12.3 were used for the analysis (MedCalc Software, Mariakerke, Belgium). The level of reliability was assessed using Cronbach's alpha, for which the recommended cut-off criterion for the co-efficient alpha is 0.70.31 In this study, missing data was found in the responses of only one of the caregivers, for whom three CSDD items were missing. These missing items were then replaced using the lowest score (zero), as suggested by Leontjevas.13
RESULTS
The demographic data, percentages of MDD diagnosis and CSDD scores are described in Table 1. Twenty-five of the 84 participants (29.8%) were found to have MDD and 35 (41.7%) were found to have cognitive impairment. There was no difference found in terms of the gender, marital status, years of education, and cognitive status of the respondents from the depressed and non-depressed groups; however, the CSDD scores were higher in the depressed group than in the non-depressed group (mean±SD, 13.60±3.66, and 4.64±3.17, p<0.001 respectively). At the same time, CSDD scores were higher in the cognitively impaired group than in the cognitively intact group (mean±SD, 8.74±5.30, and 6.29±5.07, p=0.012 respectively), though this is not shown in the table.
Cronbach's alpha for the whole group was 0.87, while for patients, caregivers, depressed and non-depressed respondents the scores were 0.84, 0.86, 0.86 and 0.86 respectively (Table 1 and 2).
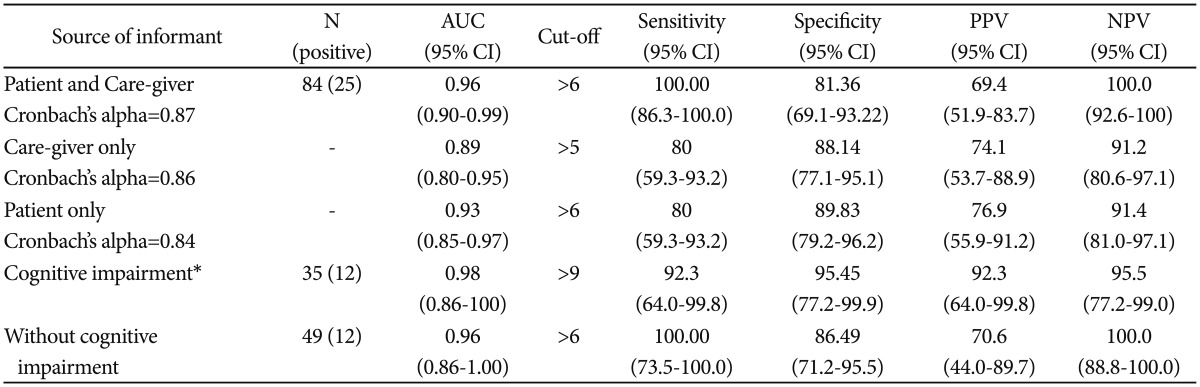
Comparing ROC curve analysis with cut-off scores according to cognitive status; and according to the source of informant
Validity of CSDD as against DSM-IV criteria using MINI
As shown in Table 2, when using DSM-IV, for all subjects the AUC for the CSDD tool was 0.963 (SE 0.0175; 95% CI 0.897-0.992), while for a cut-off of >6, it yielded a sensitivity of 100%, a specificity of 81.36% - with a positive predictive value of 69.4%, and a negative value of 100%. When looking at the ROC curve analysis - according to cognitive function, the CSDD yielded an AUC of 0.976 (SE 0.022; 95% CI 0.87-1.00) and 0.962 (SE 0.046; 95% CI 0.79-0.98) for the cognitively impaired and non-cognitively impaired groups respectively.
When comparing the ROC curve analyses of the caregivers and patients, it was found that the caregiver CSDD yielded an AUC of 0.89 (95% CI 0.803-0.948), while the patient CSDD yielded an AUC of 0.929 (95% CI 0.851-0.973).
Table 3 shows the different cut-off scores and coordinates for the CSDD ROC curve, using the standard protocol in which information from both patients and caregivers was used and the final scores for each item were based on the interviewer's judgment. At the cut-off score of >6, the Youden index J was at its highest, whereas at a score of >14, specificity was at its maximum.
DISCUSSION
Overall, the results demonstrate that the CSDD was able to detect MDD in the elderly, and especially in those with cognitive impairment. Our results seem to sit in the middle when compared to the findings of previous studies in this area, which have produced AUC figures ranging from 0.7 to 0.99.17 When compared to a previous Asian sample from Japan,32 we achieved a similar cut-off score using DSM-IV, but with a different setting. The results from our study were similar to those from Japan, indicating that nurses may be a good substitute for caregivers when they are the only source available for diagnosis.
These findings have been endorsed by a recent report produced by Leontjevas et al.,13 in which the CSDD was found to be better at ruling-out rather than ruling-in depression due to a low PPV. We yielded the same cut-off score as that study (>6); however, our Thai version showed a different AUC, which has to do with the different procedures used in the studies, for in our study the same rater administered both the MINI and CSDD tools, even though interviews were conducted on different days. This may have led to the high AUC scores; however, high AUC scores were also obtained in the Japan study, for which it is not clear how the ratings were used. We generated the same cut-off score as Lim et al.16 in their study of Korean subjects, even though the diagnostic criteria used in each study were different. Interestingly, they found a higher level of specificity than sensitivity in their study, which may have been due to differences in the sample characteristics, as their study was not conducted in a nursing home or long-term care home setting.
As found in the previous studies, CSDD showed a good internal consistency here, with the Cronbach's alpha being good for all items (0.87)13,33- covering both the patient and caregiver samples; the depressed and non-depressed groups.
Since the aim of this study was to focus on MDD, a cut-off of 6 or lower could be used to rule out major depressive episodes (MDE) without missing depressed residents. As the CSDD is a time-consuming tool to use, in the future it may be of benefit to use it to diagnose MDD without adding any further measurements. The generation of higher scores could then be used for diagnosis purposes; for example, a score of 14 or more may suggest MDE without including non-major depressive cases, as in this study (Table 3). Alexopoulos et al.30 suggested that scores above 10 indicate probable major depression, scores above 18 definitely indicate major depression, while scores below 6 as a rule are associated with the absence of any significant depressive symptoms.11,34
How else can we make use of the CSDD in a long-term care setting? Snowdon et al.15 discovered that routine use of a screening tool to identify depression in nursing homes is beneficial, particularly in cases of dementia. We agree with Snowdon4 that dementia with depression is more common in nursing home or LTC facilities than elsewhere; therefore, using the CSDD as an outcome measure to monitor changes in symptoms, so that residents with high CSDD scores may subsequently receive antidepressants, is recommended, even though the CSDD is commonly considered a screening rather than a diagnostic tool. It is not only the incidence of depression in LTC facilities that has been under detected - there has also been little research into the effectiveness of antidepressants as compared to psychosocial interventions in LTC facilities or nursing homes. Moreover, as claimed by Bharucha et al.35 and Blanchard et al.,36 psychosocial intervention in LTC facilities has also been little studied and under-utilized. In light of this, there is much more to explore in terms of the prevalence of depression among dementia patients in LTC facilities, and the CSDD will be an important tool in this process, one whose use should be promoted. CSDD can, not only establish the presence of depression, but also measure the effectiveness of any interventions given in such a setting.
This study did have some limitations. First, the sample size was relatively small, which precluded precision in terms of the point estimates and the study's power to detect the true discriminatory ability of any measure. In addition, a test-retest was not performed to ensure reliability.
In conclusion, the CSDD is a valid tool for measuring depressive disorders among residents in a long term care setting, those both demonstrating and not demonstrating cognitive impairment. Therefore, it appears that this Thai version of the CSDD is suitable for screening purposes, and may be used to detect depression in a Thai long term care home setting.
Acknowledgments
We owe a great debt of gratitude to Ms. Kanlaya Kaewsom, our former research nurse, and all the residents and caregivers at TWDCOP for their cooperation with the data collection activities.

